When you are with your child in the hospital, it may be difficult to know what to expect from him or her. Is it normal for my child to cry? Why are some parts of this so much harder than others? How do I know if my child is reacting the way that they are supposed to? And what do I do to help?
What is important to remember is that the hospital is a brand new environment, full of novel and potentially frightening experiences for your child. There is no right or wrong way for children to react to the things they see, hear and feel while they are in the hospital. A Certified Child Life Specialist (CCLS) has specialized training in child development, which provides them with expertise in how children react to hospitalization at each developmental stage. This allows the CCLS to complete two essential functions. 1. To consider what a typical cognitive and emotional reaction is for the child (assessment) and 2. To provide psychological, social, and developmentally appropriate support that will help the child to cope well during their time in the hospital (intervention). Considering a child’s stages of social and emotional development is helpful when breaking down how a child may react to the hospital environment. Although hope, will, purpose, competence, and fidelity are each building blocks that have a place in the schedule of children’s social and emotional development, it is important to remember that this speaks to children en mass and that each child develops at an individualized pace. Your child may spend more time in one stage than another, and that is okay. The goal, or optimal outcome, is for children to master each of these stages. Utilize the following descriptions below to determine where your child is in the schedule of their social and emotional development, since you know your child best!
Trust vs. Mistrust
0-1 years/Infancy
Building trust in children nurtures hope, which supports their sense that they can trust the world around them.
Infants rely on their caregivers to meet their physical and emotional needs in a consistent and caring way (Halverson, 1998). When thrust into the unfamiliar hospital environment, with a large number of strangers who have now become caregivers, infants can face separation issues, which exist on a spectrum ranging from protest to despair then to detachment. Protest is characterized by the child crying loudly, screaming for his or her caregiver, refusing attention from others and being inconsolable in his/her grief. Despair can be seen as the child stops crying, appears less active, is disinterested in play or food and withdraws from others appearing sad or lonely. Finally, a child facing detachment may appear to have adjusted to the loss, becomes more interested in surroundings playing with others. These behaviors do not demonstrate adjustment, rather the result of resignation. The child has detached him or herself from their caregiver in an attempt to cope with emotional difficulty. Infants can also face over/under stimulation by the hospital environment. Often children will attach to a material object and may need a transitional toy/object to help enter a new environment.
A CCLS will advocate for the caregiver taking an active role as part of their child’s care team and establishing a firm routine. Giving caregivers a responsibility helps them to feel included in the hospitalization process. Caregivers can develop feelings of guilt and inferiority as they watch other adults taking over the care of their child. A CCLS will help families to feel more involved in their child’s care, ensuring the infant maintains a strong attachment to their caregiver.
Autonomy vs. Shame & Doubt
1-3 years/Early Childhood
Nurturing autonomy promotes will in children and supports their sense it’s okay to be who they are.
Toddlers begin to explore their surroundings during these ages, using their parents as a strong base of security. If the caregivers provide encouragement and patience, children gain autonomy at this age and become capable of satisfying some of their own needs. For example, feeding, washing or dressing themselves. Highly restrictive caregivers may instill the child with a sense of doubt and make them reluctant to attempt new challenges. It is important at this age to remember not to demand too much too soon of your child, allowing him or her to complete the tasks of which they are capable and continuing to reinforce even their unsuccessful attempts at new challenges.
In the hospital environment, toddlers have a strong fear of abandonment at this age thinking their caregiver may leave and not come back. There can be an increase in negative and/or aggressive behaviors in response to this fear. In the hospital setting, regression is common as a reaction to stressors. For example, your child may return to bedwetting despite potty training success, demand for a bottle, or refuse to eat or nap. Most notable for a CCLS is the fear children have at this age of bodily injury or pain and the limited understanding they have of their bodies. Often small, “painless” procedures can be traumatic for this age group. They fear “people who inflict pain” often anyone they identify as a member of the medical staff.
A CCLS knows communication at this developmental stage is essential. Children must receive preparation/education regarding an upcoming medical experience or procedure. A CCLS accomplishes this through the most critical coping skill at this age: play. A CCLS would engage a toddler in a medical play session which includes not only a toy doctor’s kit, but also manipulating real medical equipment to provide the child with rehearsal of all of the steps to come. Treasure chests and rewards are strong motivators for this age group and can provide a child with a sense of accomplishment after completing a difficult hospital experience.
Initiative vs. Guilt
3-6 years/Early Childhood – Beginning of School Age
Nurturing initiative promotes purpose in children and supports their sense that it is okay for them to move an act as they do.
At this age children are learning basic skills and principles: a round ball will roll, things that fall go up and not down. Children learn to count and want to be in control as they begin to complete actions for a purpose. Confusion can present as children start to feel guilt over things that logically should not cause this emotion. Part of this stems from reality and fantasy not being distinguishable at this age. In the hospital, children at this age are threatened by bodily injury including fear of mutilation and loss of bodily parts. Misconceptions are highly common at this age as illness and medical procedures can be perceived as punishments. Fantasy and magical thinking make providing explanations of these ideas more difficult. Regression can be seen with exhibition of more toddler-like behaviors.
A CCLS will work to explain things in concrete terms, utilizing sensory aspects, always explaining to a child how it will feel, smell, look, etc. Medical and expressive play is crucial at this age as the CCLS will ask the child for feedback. Often the child will be asked to play out the information they have just learned. This will allow the CCLS to receive feedback from the child about what he/she learned and clarify any misconceptions present. Often this includes explaining to a child that hospitalization is not punishment. A CCLS will work to help the child increase their understanding of the body and its function and clarify any of their fears related to examination of the body. A CCLS will also emphasize that the child is able to verbalize his or her fears or concerns it is okay for the child to cry, yell and express discomfort. A CCLS will provide positive reinforcement while also providing limits and structure. For example, if something hurts it is okay to cry, but it is never okay to hit mommy or daddy just because you are upset. Consider this medical play session completed with a 4 year old named Susie.
I approach a 4 year old named Susie who is sitting in a chair in the Infusion Room covering her face with a fuzzy blanket her family had taken with them from home. Mom and dad sit alongside her looking visibly anxious and uncomfortable. I kneel down to Susie’s level and introduce myself to the family. I explain that I am the child life specialist in the Infusion Room and my job is to teach Susie about her special blood test today. I begin to ask Susie about herself, how old she is and what kind of toys she likes to play with. Susie removes the blanket from over her face, but still looks a little unsure of this new environment. I take out my preparation kit for medical play, showing Susie the teddy bear I have inside.
I explain, “This is my teddy, he helps me teach kids about what happens when they come to this room.” Susie sees the toy doctor’s kit I have with me and begins to play with the stethoscope, putting it up to the teddy bear. I positively reinforce this correct use of the medical equipment. As we continue to play with the toy doctor’s kit, I begin to slowly incorporate pieces of real medical equipment into our play. I introduce her to my “orange noodle” which the adults call a tourniquet. I show her how we can tie it to teddy’s arm to help the thin, blue lines called veins in our arms to show up a little bigger.
Susie continues to actively engage in the session, manipulating the medical equipment that I provide to her. She wipes the teddy’s paw with the alcohol swabs I have given her. “These are wet!” she exclaims which provides me with an opportunity to discuss sensory experiences. I explain to her that when we use the alcohol swabs on her arm, they will feel wet and probably a little cold too. I progress through our medical play to explain that we need to use a “helper poke” to put the IV straw into Susie’s arm. “I don’t want a shot!” she tells me. I begin to clarify misconceptions. I show Susie the tiny, plastic IV straw that we can use to test our body’s blood and to give it medicine and explain this is different than a shot.
Susie looks doubtful so I hand Susie the small IV straw and ask her to try to see the hole. “It’s too small to see!” she tells me. I told Susie how the small hole that we can barely see helps the nurse to test her blood more than one time throughout the day, without having to do more than one poke. I show Susie how the helper poke gets “locked away” once it is done helping put in the straw. We decided to practice putting the IV straw into the teddy’s paw. I think the teddy is going to cry” she tells me. This piece of feedback helps me to assess that Susie is fearful for the IV insertion and that she believes it is going to hurt. I validate Susie’s concerns and talk about things we could do to help teddy be less scared and to make the poke part hurt less.
Susie told me teddy would be less scared if he could sit on her lap and hold her hand. I reinforced this as a positive idea for teddy. I told Susie how taking deep breaths can help relax our bodies which makes the poke part hurt a little less. Susie took a big breath in and out. “That was a nice, slow deep breath!” I told her. Susie said she thought teddy would like us to count to 3 before we did the poke part too. As she came up with ideas to help teddy, Susie actively took part in developing her own individualized coping plan.
Susie’s nurse arrived to begin the IV insertion. Susie was able to verbalize out loud the steps she remembered from the medical play. For example, she said, “oh the noodle!” when the nurse tied the tourniquet around her arm. Susie became very fearful and anxious just before the poke. When the needle went in to insert the IV straw, Susie cried and said, “this hurts, I don’t like this!” I asked Susie what happens to the helper poke after it puts in the straw. Through her tears, Susie told me, “it gets locked away!” I was able to engage Susie in practicing her deep breathing for the remainder of the IV insertion.
Susie reacted in a developmentally appropriate way to her IV insertion. The medical play helped to prepare her for each step. Susie cried during her poke, which is a reasonable and expected reaction for any 4 year old receiving an IV. What I consider as a CCLS, is that Susie was able to redirect to conversation with me and provide me feedback about what step was next. Susie also was able to calm down by taking deep breaths, which a CCLS describes as “returning to baseline.” I reinforced Susie’s positive coping behaviors by telling her how proud I was of her holding still and taking deep breaths. This focuses on the positive things she did to help the IV insertion go well to promote her doing these things again in the future. Susie is an example of a patient who participated actively in her own treatment merely by taking part in play.
Industry vs. Inferiority
6-12 years/School Age
Nurturing industry promotes competence in children and supports their sense that they can make it in the world around them.
Children at this age are eager to learn and accomplish more complex skills, further developing themselves as individuals. They tend to form values and recognize differences between themselves and others at this age. They manage their personal needs independently, working hard at being responsible. In the hospital setting, this growing sense of wanting responsibility and accomplishment makes children want to take part in their own care. A CCLS will advocate for children participating in medical procedures whenever possible. For example, selecting an arm for an IV insertion, pushing buttons on machines, taking off their own band-aids, etc.
Misunderstandings that occur at this age stem from children taking information quite literally. Figures 1.1-1.3 show drawings completed from children in this age group after being presented with medical terminology. From this example, you can see that a “cat scan” could be misinterpreted to literally mean scanning a cat. Concerns about waking up from surgery is a common issue as children often associate “being put to sleep” with the ending of life of their pet cats or dogs. Children at this stage also have a fear or not being “normal” or fitting in with their friends, which can lead to a decrease in self-esteem. Children tend to fear not being well again or their body being altered or in pain from medical procedures or surgeries. At this age, it is common for anxiety about illness and death to develop. Children have many questions regarding hospitalization based on this anxiety.
A CCLS will provide a child with as much information and choices as possible to allow the child to gain mastery over the experience and feel prepared. A CCLS will explain words that may have double meanings and use less threatening language. For example, rather than “the doctor will cut/slice” saying “the doctor will make a small opening, smaller than a paper clip.” A CCLS must consider any past negative hospitalization experiences the child may have had. Providing structure through limit setting and routine is important for children at this age. A CCLS will also encourage peer support through phone calls and visits from friends during long term hospitalization. A CCLS serves as an advocate for patient with other medical staff, often reminding them to directly address children at this age rather than their parents and to provide them with choices and opportunities for participation.
Figure 1.1 A child’s perception of the word “cat-scan”

Figure 1.2 A child’s perception of the word “stretcher”
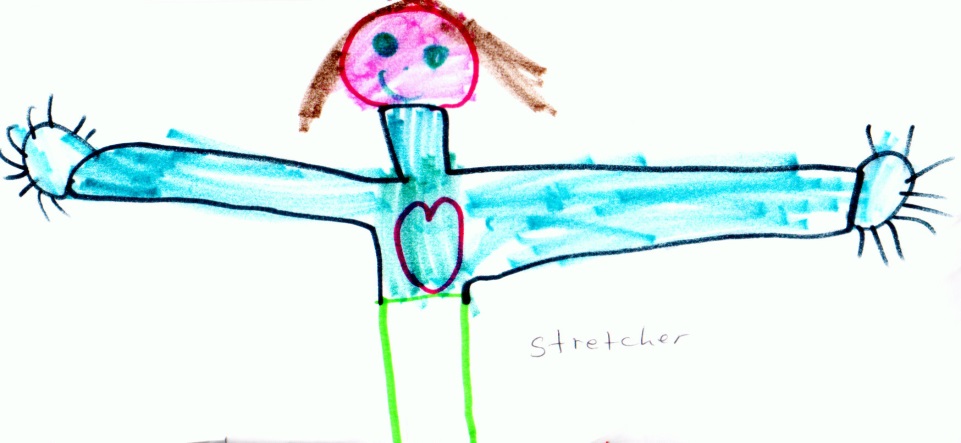
Figure 1.3 A child’s perception of the phrase “stool collection”

Identity vs. Role Confusion
through 18 years/Adolescence
Nurturing a child’s personal identity promotes fidelity in them and supports their sense of who they are and who they can be.
This age marks the transition from childhood to adulthood, which can result in role confusion as adolescents determine how they will fit into the adult world and what hospitalization means for their future. Some teens experience mixed ideas and feelings about what their role as an adult will be and begin to experiment with a variety of behaviors, activities and hobbies. They will test the limits of their personal values and belief systems as well. Adolescents can be very self-conscious and focused on privacy. This causes issues in the hospital setting as teens have a hard time revealing personal information in front of their caregivers. They worry about being separated from their peers and being in close quarters with their family members. Significant issues regarding altered body image, loss of privacy and lack of control emerge in the hospital setting. A CCLS will provide teens with as much control as possible to respect their internal struggle of wanting to emerge as an adult and being treated as a child. A CCLS will utilize the same words the teen uses for his or her body and medical terminology. A CCLS will incorporate their words whenever possible and then educate them on sophisticated terminology. A CCLS advocates strongly to the medical team that teens should never be treated as children and should be involved in the development of their own care plan. A CCLS will explain the importance of medical staff asking permission to enter a teen’s hospital room and providing them with a private space.
Being in the hospital setting can be overwhelming for any family. Knowing what types of behaviors could be present in your child can help you to feel more prepared for medical experiences. Continuing to offer your child opportunities to process the information they are learning while in medical settings can help your child to adjust and develop coping skills. It may be normal for your toddler to cry during a “painless” procedure or for your school age child to think they won’t wake up from surgery despite you explaining that they will multiple times. It is common for parents to worry about these reactions, thinking their child is not coping well or processing information. However, these types of reactions demonstrate that the child is responding to the hospital environment in the best way they know how. Your job as the caregiver is to provide your child with love and support throughout their medical experiences. The CCLS will help your family to navigate through each experience, providing developmentally appropriate support each step of the way!